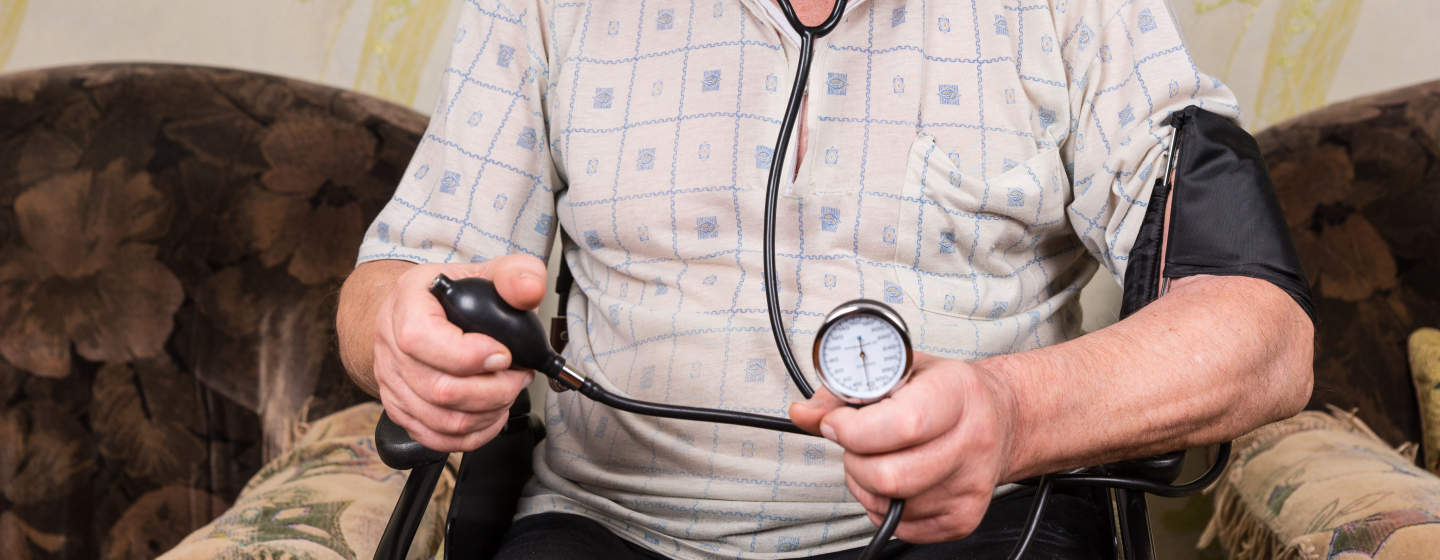
An increase in blood pressure (BP) is a natural part of ageing, and is caused by arteries stiffening and hardening over time. However, the effects of this natural increase can be exacerbated by the long-term build-up of unhealthy lifestyle habits, such as low levels of exercise, poor diet and drinking too much alcohol. More concerningly, trends in blood pressure in youth can impact upon BP later in adulthood. A recent report in the journal Circulation: Cardiovascular Imaging showed that for every 10-point increase in systolic blood pressure – for example, from 120 to 130mmHg – between the ages of 36 and 69, myocardial perfusion (efficient blood flow to the heart) dropped by up to 6% by the age of 77. This led to an increased risk of heart attack, stroke or heart failure. The largest rise in BP was between the ages 43 and 63, which underscores the importance of keeping an eye on your BP during midlife to maintain your heart health when older.
However, whilst we often think of blood pressure as one static measurement, it’s actually much more complicated than that, and blood pressure follows your natural circadian rhythm. This short article will look at how your BP changes throughout the day, outline exceptional cases where fluctuations can be an issue, consider the impact of antihypertensive medications, and explain why 24/7, year-round monitoring of your BP can help uncover health issues that may otherwise remain hidden – empowering you to take better care of your heart health.
Blood pressure throughout the day: not a static measurement
Your circadian rhythm, or ‘internal body clock’, is a 24-hour cycle that influences your wake/sleep pattern, telling you when to go to sleep and when to wake up. It also feeds into many other body processes, including your hormones, digestion and body temperature, affecting your physical, mental and behavioural changes throughout the day.
In fact, while we often think of blood pressure as a single, static number, it’s actually constantly fluctuating in-line with your wake/sleep cycle, or your circadian rhythm. In a healthy individual, BP will start to rise a few hours before waking, continuing to rise until around midday, which is when it’s at its highest. It then tends to fall during the late afternoon into the evening, and overnight it should be at its lowest, between 10 and 20% lower than your daytime average.
There are several irregular patterns of blood pressure that are sometimes seen in patients, which can include:
- high blood pressure during the night;
- high blood pressure early in the morning;
- a drop in blood pressure of less than 10% overnight (non-dipping blood pressure)
These irregularities can be indicative of underlying health conditions, like poorly controlled hypertension, obstructive sleep apnoea, kidney disease, diabetes and thyroid disease. Poor sleep may also be a contributing factor.
Fluctuating BP is normal, but there are some exceptional cases
It’s likely that you already know the common factors that affect blood pressure long-term, which include age, obesity, lack of exercise, poor diet and genetic history. However, even in individuals without hypertension, BP fluctuation can be substantial during moments of physical or emotional stress, sometimes without a clear provocation.
There are five circumstances under which the changes in BP, potentially causing hypertension, can be a clinical issue:
- White coat hypertension (and masked hypertension)
- Labile hypertension
- Paroxysmal hypertension
- Orthostatic hypertension
- Patients with underlying health conditions
White coat hypertension
White coat hypertension is a type of BP increase that occurs at the time of measurement, often at the doctor’s, and is usually due to anxiety over the measurement being taken. This type of hypertension is short-lived, but can still cause damage to key organs such as the heart, and is associated with development of sustained hypertension. It’s actually fairly common, which is reflected in the NHS’s guidance for talking BP. The NHS states that your blood pressure is usually considered high if it’s either:
- 140/90 or higher when checked by a healthcare professional
- 135/85 or higher when checked at home
The opposite of this is ‘masked hypertension’, where patients exhibit normal BP measurements within a clinical setting, but high ones at home. This condition is estimated to affect about 10% of the general population, but is hard to diagnose and, like other forms of hypertension, can lead to organ damage and increased risk of adverse cardiovascular events.
In both cases, the use of a discreet, wearable device that passively takes BP measurements, such as the Hilo Band, may be a useful tool for both patient and clinician.
Labile hypertension
Between the 1960s and 1980s, the term ‘labile hypertension’ was used as a category for patients who had BP in the range between normal (less than 120/80 mmHg) and high (over 140/90 mmHg). This term is no longer used for patients in this category, and today those patients would be categorised as having ‘elevated BP’, which then transitions to a diagnosis of hypertension at measurements of above 140/90 mmHg.
However, the term ‘labile hypertension’ is still used, but nowadays, it is defined as a condition where the increase in BP is “provoked by obvious stress or anxiety; they may be asymptomatic or have hyperadrenergic symptoms” i.e. you may not notice any change or symptoms (asymptomatic), or you may feel a sudden rush of adrenaline.
Paroxysmal hypertension
While labile hypertension often has a clear trigger, paroxysmal hypertension – also called pseudopheochromocytoma – usually occurs in the absence of emotional distress and ‘comes out of the blue’. These events can be short-lived, or in some cases last for days. However, while their onset may not have a clear cause, in this case BP elevation is accompanied by physical symptoms including headache, palpitations, flushes or weakness.
Orthostatic hypertension
Orthostatic hypertension (OHT) is a condition that is characterised by a sudden increase in blood pressure when a person stands up. It is common in patients both with and without a hypertension diagnosis, but its presence in younger persons can result in hypertension in later life, and in older persons can lead to an increased risk of morbidity (the likelihood of suffering from an illness) or mortality (likelihood of death) from cardiovascular conditions.
The opposite condition, orthostatic hypotension, is characterised by a sudden drop in BP upon standing (postural hypotension is a sudden drop in BP when changing position more generally, rather than specifically standing). This can cause feelings of dizziness or fainting, and is more common in people over 60, especially those who have been confined to bed rest, and can happen more frequently in the morning.
Patients with underlying health conditions
Although a degree of fluctuation in BP is perfectly normal, studies have shown that increased long term BP variability may be associated with an increased risk of heart attack, stroke and atrial fibrillation.
Hilo Band: An aid to identifying hypertension in difficult cases
All the hypertensive conditions outlined are difficult to diagnose, either because they’re transient, measuring BP induces anxiety leading to higher numbers or, inversely, the higher numbers are only seen outside a clinical setting. In these cases, using a Hilo Band can give insight into what your BP does over the day, and, importantly for the case of white coat hypertension and masked hypertension, you won’t even know when the measurement is being collected.
The Hilo Band takes numerous cuffless readings throughout the day – up to 25 within 24 hours – which is exactly what is needed to identify masked hypertension and white coat hypertension. Furthermore, the companion app presents data in an easy-to-read format, allowing you to quickly identify trends and patterns in your BP measurements throughout the day.
It should be noted that labile, paroxysmal and orthostatic hypertension are harder to diagnose, and the Hilo Band may not pick up on these events if they are short-lived or occur while you are moving.
Daily variation when on BP medication
If you have hypertension, then you may be prescribed BP-lowering medication. Often a combination of medications are needed to adequately control blood pressure. Your healthcare professional will advise you when best to take your medication and if you have any concerns it is best to address these with your physician as the dose, the dose timing or the medication itself may need to be adjusted.
While taking these medications, it is still normal for your BP to vary across the 24-hour period, in-line with a normotensive individual not taking medication: rising a few hours before waking, continuing to rise until around midday, falling in the late afternoon and evening, then at its lowest overnight. Keeping a medication calendar, either on paper or in your Hilo App, is a good way of ensuring medication adherence.
It’s key that if you think that there are issues with your medication you should always speak to a doctor before making any changes, and you should never stop taking medication without consulting with your doctor.
If you’d like to find out more about blood pressure and topics related to blood pressure, sign up to the Hilo newsletter.
Get an overview of your BP with the Hilo Band
We often consider blood pressure to be a static value, likely because when data are collected using a traditional inflatable cuff, you only get a snapshot. However, by only taking one measurement you’re only getting a small part of the story, and the variations of BP throughout the day and night can give a more rounded view of your overall health.
The Hilo Band changes that, giving you clarity and overview 24/7, 365 days per year. The medical device – which is backed by European and FDA approval, more than two decades of research, and data from over 120,000 registered users worldwide – uses an optical sensor to measure the pulsation of the arteries beneath the skin, analyses the ‘shape’ of the pulsation and extracts the information needed to give you BP measurements day and night. The automated, continuous operation allows you to achieve up to 25 measurements per day, giving you a comprehensive overall picture of your blood pressure and its range. In addition, the Hilo App ensures that all data are presented clearly and simply, as well as being easy to share with your doctor.
While for those with normal BP measurements this may just satisfy your interest, in other cases it may help identify underlying medical conditions that haven’t been picked up previously, such as masked hypertension or a ‘non-dipper’ profile. It can also allow you to see the results of any medical interventions in real-time, for example if you’re taking BP-lowering medications or setting-off on a healthy lifestyle (the app now allows you to see your step count and sleep quality as standard).
Disclaimer: This article is for informational purposes only and does not contain, nor replace, medical advice. The information in this article is not intended to diagnose, treat, cure, or prevent any disease. Talk to a qualified medical professional before making any changes to your health regimen, medication included.
Sources
Could too low blood pressure in old age increase mortality? British Geriatrics Society. https://www.bgs.org.uk/could-too-low-blood-pressure-in-old-age-increase-mortality (Accessed March 2026)
Causes of high blood pressure. Blood Pressure UK. https://www.bloodpressureuk.org/your-blood-pressure/causes/ (Accessed March 2026)
C.-C. Topriceanu, M. Webber, H. Shiwani, F. Chan et al. (2025). Higher Life-Course Blood Pressure Associates With Reduced Myocardial Perfusion in Older Age: Insights From MyoFit46, Circ. Cardiovasc. Imaging, 19, e019105. https://doi.org/10.1161/CIRCIMAGING.125.019105
Myocardial perfusion scan. British Heart Foundation. https://www.bhf.org.uk/informationsupport/tests/myocardial-perfusion-scan (Accessed March 2026)
Blood pressure must be controlled in midlife before irreversible damage is done. British Heart Foundation. https://www.bhf.org.uk/what-we-do/news-from-the-bhf/news-archive/2020/september/blood-pressure-must-be-controlled-in-midlife-before-irreversible-damage-is-done (Accessed March 2026)
Does the time of day affect blood pressure? Hilo. https://hilo.com/uk/art/blood-pressure-time-of-day/ (Accessed March 2026)
H.-J. Choi (2012). Blood Pressure Variability and Its Management in Hypertensive Patients, Korean J. Fam. Med., 33, 330. https://doi.org/10.4082/kjfm.2012.33.6.330
E. J. Filippone, G. V. Naccarelli, A. J. Foy (2025). Controversies in Hypertension VI: Paroxysmal Hypertension, Am. J. Med., 138, 1330. https://doi.org/10.1016/j.amjmed.2025.04.023
Getting a blood pressure check. Blood Pressure UK. https://www.bloodpressureuk.org/your-blood-pressure/getting-diagnosed/getting-a-blood-pressure-check/ (Accessed March 2026)
White coat hypertension: when blood pressure rises in a medical setting. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/expert-answers/white-coat-hypertension/faq-20057792 (Accessed March 2026)
Blood pressure test. National Health Service (NHS), UK. https://www.nhs.uk/tests-and-treatments/blood-pressure-test/ (Accessed March 2026)
T. G. Pickering, K. Enguchi, K. Kario (2007). Masked Hypertension: A Review, Hypertens. Res., 30, 479. https://doi.org/10.1291/hypres.30.479
Hilo Band. Hilo. https://hilo.com/uk/blood-pressure-monitor/ (Accessed March 2026)
Blood Pressure Table by Age. Hilo. https://hilo.com/uk/art/blood-pressure-by-age/ (Accessed March 2026)
Understanding Blood Pressure Readings. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings (Accessed March 2026)
S. J. Mann (2009). The Clinical Spectrum of Labile Hypertension: A Management Dilemma. J. Clin. Hypertens., 11, 491. https://doi.org/10.1111/j.1751-7176.2009.00155.x
D. Mamilla, M. K. Gonzales, M. D. Esler, K. Pacak (2019). Pseudopheochromocytoma, Endocrinol. Metab. Clin. North Am., 48, 751. https://doi.org/10.1016/j.ecl.2019.08.004
J. Jordan, F. Ricci, F. Hoffmann, V. Hamrefors, A. Fedorowski (2020). Orthostatic Hypertension: Critical Appraisal of an Overlooked Condition, 75, 1151. https://doi.org/10.1161/HYPERTENSIONAHA.120.14340
Orthostatic-hypotension. National Health Service (NHS), UK. https://www.oxfordhealth.nhs.uk/wp-content/uploads/2011/03/OP-111.15-Orthostatic-hypotension.pdf (Accessed March 2026)
Low blood pressure (hypotension). National Health Service (NHS), UK. https://www.nhs.uk/conditions/low-blood-pressure-hypotension/ (Accessed March 2026)
Blood pressure variability is a major predictor of heart attack and stroke risk. Imperial College London News. 31st January 2024. https://www.imperial.ac.uk/news/251055/blood-pressure-variability-major-predictor-heart/ (Accessed March 2026)
How often does the Hilo Band take a BP reading? Hilo. https://support.aktiia.com/en/articles/80000932099-how-often-does-the-hilo-band-take-a-bp-reading (Accessed March 2026)
Medicines for high blood pressure. Kidney Care UK. https://emedia2.nhs.wales/wrcn/assets/Medicines/Medicines_for_high_blood_pressure%20KCUK.pdf (Accessed March 2026)